If you deal with the painful and potentially debilitating gut symptoms that are associated with IBS, I know how frustrating it can be when you might hear the condition dismissed or painted as being something that’s mostly ‘in your head.’
The reality is, IBS is a very real condition and the more we find out about the mechanisms that underpin it, the more that’s made crystal clear.
So what does the recent research show?
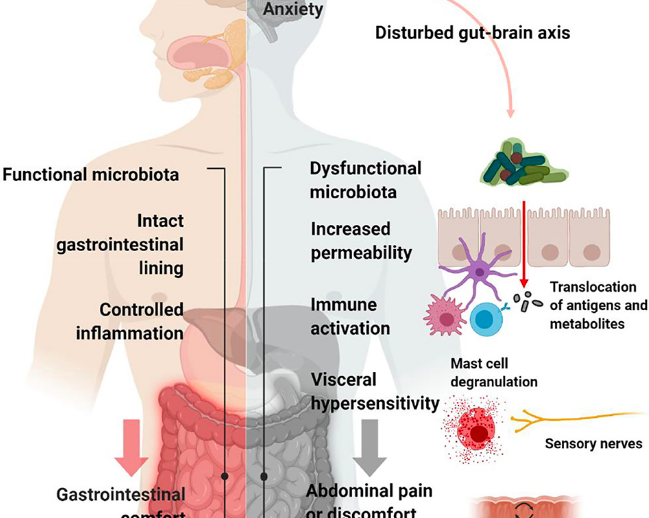
Take a 2021 study which included over 50,000 people. This found that the same genes that put you at an increased chance of developing IBS also appear to up your risk of mood disorders, including anxiety, depression and insomnia. Now that’s not to say that one causes the other – rather, that the issues share similar genetic roots – but it does stress the reality of the gut:brain axis in IBS.
Another interesting highlight from the same research is that a significantly higher proportion of people with IBS recalled taking long term or recurrent courses of antibiotics as children. This, like you’ve probably guessed, can result in alternations in the gut microbiome, which in turn can impact the sensitivity of your gut lining, which is one of the key observations in IBS. The researchers also found that people who have had surgeries such as appendix or gallbladder removal are more likely to develop IBS, really highlighting the physical reality of the condition.
More recently, a team of researchers from Belgium discovered a potential role of the immune system (one that’s overactive) in IBS. Up until now, the immune system wasn’t thought to be involved in IBS. In fact, the key mechanism by which food triggered gut symptoms was believed to be solely down to the irritation of the gut lining by bacteria fermenting food, which produces gas and an array of chemicals. But this new research pointing to the immune system, at least in some IBS suffers, is very exciting and creates new possibilities for the treatment of IBS. My team at King’s College London is also currently investigating individualised dietary therapies for people with functional gut disorders (which is the category of gut conditions that IBS falls under).
Here we’re figuring out why certain foods, like beans and onions, trigger symptoms like bloating in some but not others. We’ve just finished wrapping up the intervention study and we’re now doing the data analysis, which I’ll share as soon as it’s released.
Now this is all seriously exciting yet complex, and research is on-going to figure out how best to understand and treat IBS. But rest assure, there is still plenty of simple and practical strategies that you can put in place today to help manage your symptoms as we’ll discuss.
Before you move on to the next section, it’s a good idea to confirm whether you fulfil the criteria for an IBS diagnosis if you haven’t already. This can be done by completing the ‘Is it IBS or another Functional Gut Disorder’ assessment in Eat Yourself Healthy or Love Your Gut.
Okay, so what do I do about my IBS?
So sure, a lot of research is on-going and the most effective treatment for IBS is likely yet to be discovered. In the meantime, we do have advice which has been proven (in human studies, not just animal!) to help. Try the tips below; they could well start to alleviate some of your symptoms.
The first line dietary approach
Heaps of research shows that changing what you eat and drink can help you to manage IBS symptoms. The first-line approach has been shown to achieve impressive benefits in around 50% of people with the condition and, good news, it’s something you can start on your own.
Note: to get specific, you could keep a gut diary for one to two weeks, in which you jot down if any of the below foods or drinks trigger symptoms, ahead of trying any restrictions – check out Eat Yourself Healthy or Love Your Gut for your template. If they do, follow the recommendations for said foods or drinks below:
- Alcohol: Drink no more than one standard drink a day (equivalent of around 330ml low-strength beer,
100ml wine or 25ml spirit). - Caffeine: Limit to one caffeine-containing drink/food a day, e.g. 1 single shot coffee, 1 tea.
- Spicy food: Limit chilli-containing meals.
- Fat: Limit large portions of high-fat foods, particularly those with limited nutritional value, i.e. high-fat fast food.
- Water: Drink 1.5–2 litres of fluid per day (aim for mostly water).
- Dietary fibre: Spread fibre intake evenly across the day. Aim for 2 pieces of fruit, 5 portions of vegetables, 3 portions of wholegrains and 1 or 2 portions of nuts/ seeds/ legumes each day.
- Fruit: No more than 1 piece of fruit per sitting.
- Sweeteners: Avoid all sweeteners ending in -ol
If isolating specific trigger foods and drinks and cutting back doesn’t help, you can try following ALL of the recommendations above for one to four weeks, alongside strategies like meditation and yoga. You can find a step-by-step gut-directed yoga flow and sleep protocol in my first book.
The second line dietary approach
If that doesn’t work? Then it’s time for the second line dietary approach. This involves a low-FODMAP diet. You can get dosed up on the specificities of this, including my FODMAP-lite approach (one that you can safely try on your own) on p.145 of my first book, Eat Yourself Healthy or Love Your Gut.
In terms of supplements, these three have the most evidence of helping with IBS:
- Psyllium
- Peppermint oil capsules
- SPECIFIC probiotics
Check out the book (p.154-155.) for more details on these.
There’s so much left to learn about IBS, and I’ll keep you updated as things progress. In the meantime, if you have symptoms, know that there is a route to less suffering – even if it’s not a cure just yet. You’ve got this!